Case Report Published on December 28, 2024
Misleading Mimicry - Melioidosis A Case Report
Anju Mariya Varghese1, Arjun G Menon1
1. Department of Otorhinolaryngology, Head and Neck Surgery, Amala Institute of Medical Sciences, Thrissur Kerala*
ABSTRACT
Melioidosis is an emerging infection in India, caused by the gram-negative bacteria Burkholderia pseudomallei. It is a multisystem disease and is fatal with significant mortality and morbidity. The prognosis is excellent if detected early and managed. We report a case of 15 year old female with cervical abscess who did not respond to routine antibiotic treatment and her condition worsened until proper diagnosis was made and appropriate antibiotics started. Head and neck melioidotic abscesses are often confused with cold abscesses by Mycobacterium tuberculosis especially in an endemic country like India with a huge tuberculosis burden. The treatment modalities for both is very different and if not detected early and managed appropriately can be fatal.
Keywords: Burkholderia Pseudomallei, Melioidosis, Neck Abscess
INTRODUCTION
Melioidosis, a potentially fatal disease caused by Burkholderia pseudomallei, a saprophytic Gram - negative soil and water bacterium is endemic in areas such as Southeast Asia and northern Australia.The recent increase in the number of cases being reported from areas beyond it’s endemic boundries makes it an emerging and evolving disease in other regions like India,China, Sri Lanka, North and South America.1
CASE REPORT
A 15-year-old female with no significant medical history presented with a 4-week history of persistent right-sided neck Swelling (Figure 1). The swelling has gradually increased in size despite being treated with oral antibiotics. The patient also reports mild pain over the swelling and discomfort while swallowing. There is no history of contact with tuberculosis or overseas travel. On examination a diffuse swelling located in right level 2 and 3 of the neck seen, measuring approximately 4 x 3 cm. The swelling is firm, mildly tender, and non-mobile, with no signs of local inflammation. Overlying skin is normal, pinchable, and without erythema. Laryngeal Crepitus present. The rest of the ENT examination was within normal limits. Evidence of pediculosis scalp present.
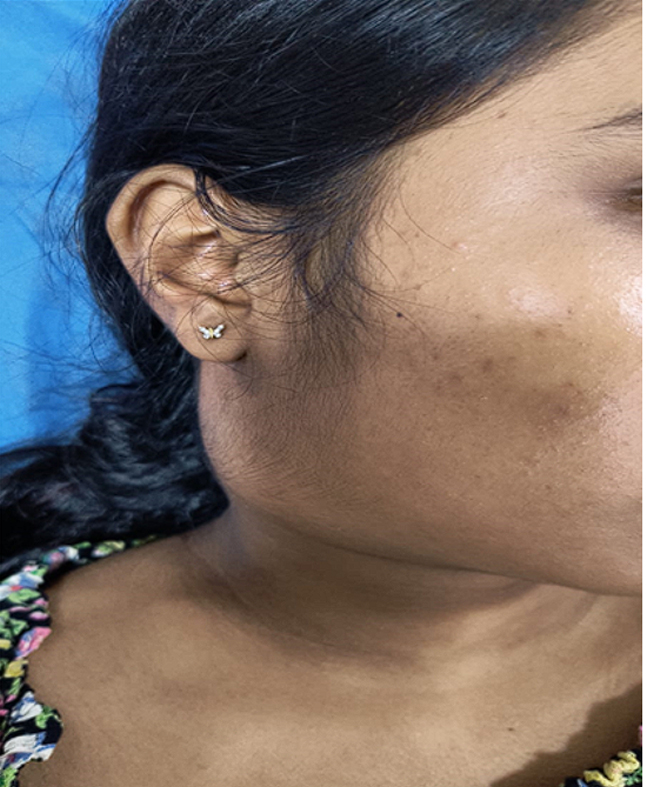
Figure 1. 15 year old female with right sided neck swelling for 4 weeks.
The patient was admitted with a suspicion of acute lymphadenitis and was started on IV antibiotics along with other symptomatic management. An ultrasound of the neck revealed a necrotic right level 2 lymph node and multiple hypoechoic nodes with absent hilum in right levels 3, 4 and 5 raising suspicion for tuberculous lymphadenitis. Peripheral smear revealed neutrophilic leukocytosis. CBNAAT did not detect Mycobacterium tuberculosis. USG-guided FNAC was performed, and the results showed a chronic inflammatory lesion with granuloma formation and suppuration. Despite being on IV antibiotics, the patient’s symptoms continued to worsen. There was an increase in pain and further enlargement of the swelling. To evaluate the extent of the disease, a contrast-enhanced CT scan of the neck was performed, which revealed a peripherally enhancing necrotic collection in the right suprahyoid region, with involvement of the right parotid and carotid space, with compression of the right internal jugular vein (Figure 2,3). The findings were consistent with conglomerate necrotic lymph node collection and most likely Tuberculosis etiology was suspected.
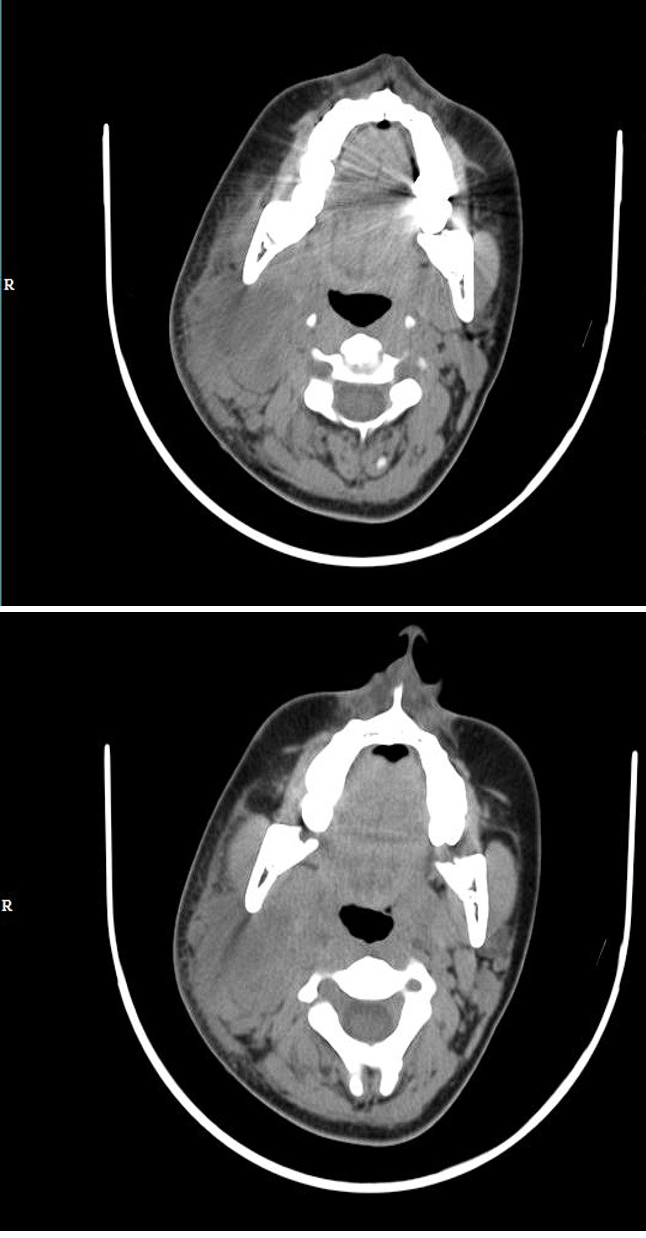
Figure 2,3. CECT NECK- A peripherally enhancing necrotic collection in the right suprahyoid region
Proceeded with right cervical lymph node Excision under GA. Pus was seen extruding from the necrotic LN and the contents of necrotic LN were scooped (Figure 4,5).
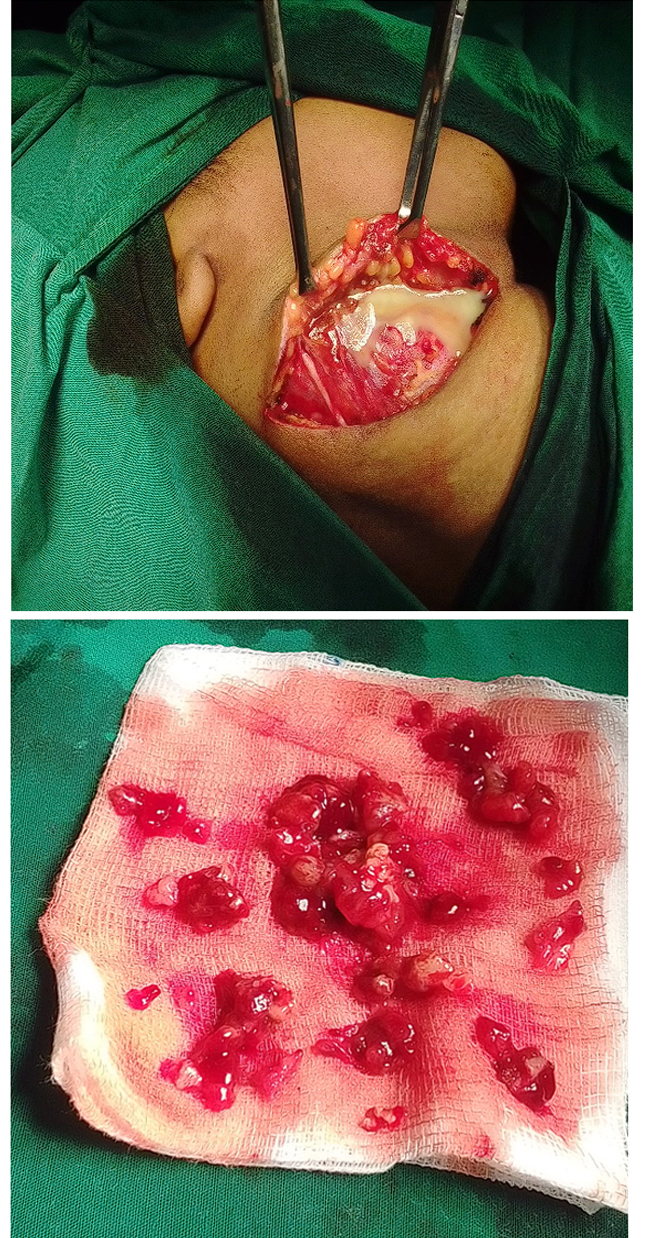
INTRAOPERATIVEFINDINGS
Figure 4: Pus seen extruding from the necrotic LN
Figure 5: The contents of necrotic LN scooped out
Pus culture and sensitivity revealed Gram negative bacteria Burkholderia pseudomallei. A Diagnosis of Melioidosis was made and she was started on Inj Ceftazidime (2GM) for 14 Days followed by Co – Trimoxazole for 4 Weeks according to the culture and sensitivity reports. Patient was relieved of all symptoms (No fever, neck swelling).
DISCUSSION
Melioidosis, also called Whitmore disease, was first described in 1912 by Alfred Whitmore and Krishnaswami .Also called “glanders-like disease.” It is caused by an aerobic, motile gram-negative bacillus Burkholderia pseudomallei, which is common in soil, water bodies.2,3 Melioidosis is endemic in Southeast Asia and northern Australia. There has been a recent increase in the number of cases being reported from India , mostly from southern states like Kerala, Karnataka, and Tamil Nadu (1–3). The key risk factors for melioidosis include diabetes, chronic alcohol use, chronic kidney disease, and chronic lung disease. It can be transmitted by bacterial inoculation or inhalation. The incidence is higher during the rainy season, as it gets transmitted by percutaneous inoculation, when individuals are exposed to wet season soils or contaminated water.2,4 Case-fatality rate is high. Now it is considered a potential bioweapon for bioterrorism.5
Clinical manifestations are of wide range. The infection can be acute or chronic, and either localized or disseminated. Clinical signs and symptoms include septicaemia, pneumonia, bone and soft tissue infections, disseminated abscesses,mycotic aneurysms, lymphadenitis, and childhood parotitisThis probably is the main reason for its underdiagnosis /misdiagnosis.2,6
Melioidosis involving the ENT (ear, nose, and throat) and head and neck regions is relatively rare. Neck mass due to melioidosis can present either as suppurative infection (acute or chronic) or as relapse.1,7 Diagnostic confusion with cold abscesses caused by M. tuberculosis in a tuberculosis- endemic country like India can occur.1,5
The diagnosis of melioidosis is typically confirmed through culture from sterile sites. Laboratory misidentification is relatively common.6
The treatment consists of intravenous, high-intensity phase and an oral maintenance phase to prevent recurrence. After the surgical drainage of the abscesses, the intravenous, intensive phase is initiated and administered for a minimum of 10 to 14 days and continued until the patient has no more fever spikes. Ceftazidime is the drug of choice. Meropenem, imipenem, and cefoperazone-sulbactam are also effective. Intravenous amoxicillin-clavulanate is also used with variable results. Eradication therapy with co-trimoxazole and doxycycline for 12 to 20 weeks to reduce recurrence is followed.6
CONCLUSION
Melioidosis is an emerging concern in India. Melioidosis is likely highly prevalent in western coastal India, yet remains greatly underestimated.1,8,9
Diagnostic confusion with cold abscesses by Mycobacterium tuberculosis in a country like India with high burden of tuberculosis is common and high vigilance and clinical suspicion is important, as the treatment modalities for both is different. Low clinical suspicion or misidentification of the organism as a culture contaminant or a Pseudomonas species is the main cause for its underreporting / misdiagnosis.1 Any patient with or without risk factors who presents with multi-system disease or abscesses should be evaluated for melioidosis especially if their condition seems to worsen despite proper antibiotic treatment.
END NOTE
Author Information
- Dr Anju Mariya Varghese, MBBS, Junior Resident,
Department of Otohrhinolaryngology.
Amala Institute of Medical Sciences, Thrissur, Kerala. - Dr Arjun G Menon, MBBS, MS
Professor, Department of Otorhinolaryngology,
Amala Institute of Medical Sciences, Thrissur, Kerala
Funding: No funding from external source.
Conflict of interest: None declared.
REFERENCES
- Mohanty S, Sarkar S, Mishra B. Melioidosis of the Head and Neck: A Case Series from Eastern India. Infect Dis Rep. 2020 Oct 29;12(3):36–45.
[Pubmed] - Dk D, N B, M D, P S, Sk M, V K, et al. A case series of melioidosis: An underdiagnosed infection. IDCases [Internet]. 2023 Jan 11 [cited 2024 Dec 23];31.
[Pubmed] - Cheng AC, Currie BJ. Melioidosis: epidemiology, pathophysiology, and management. Clin Microbiol Rev. 2005 Apr;18(2):383–416.
[Pubmed] - Currie BJ. Melioidosis: an important cause of pneumonia in residents of and travellers returned from endemic regions. Eur Respir J. 2003 Sep;22(3):542–50.
[Pubmed] - Rajinikanth J, Balaji V, Gaikwad P, Muthusami JC. Melioidosis of the parotid: the tip of the iceberg. Otolaryngol--Head Neck Surg Off J Am Acad Otolaryngol-Head Neck Surg. 2008 Nov;139(5):731–2.
- V S, Mp K, Mc H, T D, Ss M. Melioidosis and tuberculosis: dual pathogens in a neck abscess. J Laryngol Otol [Internet]. 2009 Nov [cited 2024 Dec 23];123(11).
[Pubmed] - Wk L, Gs G, K N. Melioidosis of the head and neck. Med J Malaysia [Internet]. 2001 Dec [cited 2024 Dec 23];56(4).
[Pubmed] - Vidyalakshmi K, Shrikala B, Bharathi B, Suchitra U. Melioidosis: an under-diagnosed entity in western coastal India: a clinico-microbiological analysis. Indian J Med Microbiol. 2007 Jul;25(3):245–8.
[Pubmed] - Jesudason MV, Anbarasu A, John TJ. Septicaemic melioidosis in a tertiary care hospital in south India. Indian J Med Res. 2003 Mar;117:119–21.
[Pubmed]