Original Research Published on December 28, 2024
A Prospective Study on the Clinical and Bacteriological Profile of Deep Neck Space Infection
Anjali Vinod1, Pramod Menon1, Satheesh S1
1. Junior Resident, Department of Otorhinolaryngology, Government Medical College, Thiruvananthapuram*
ABSTRACT
Deep neck space infections (DNSI) are bacterial illnesses that involve several spaces in the neck. Though the occurrence of deep neck infections has been declining since the advent of antibiotic therapy, they still occur and their diagnosis as well as treatment poses a challenge. Treatment of DNSI includes antibiotic therapy, airway management and surgical intervention. Results of various similar studies conducted in different parts of India including southern Kerala shows large variations in epidemiological pattern; hence this study was conducted to know the prevalence, pattern, source of infection, bacteriological profile and sensitivity to antibiotics of DNSI
Objectives : The primary objective was to study the clinical and bacteriological profile of deep neck space infections and the secondary objective was to study the predisposing factors, treatment outcome and complications of deep neck space infections.
Methodology : The prospective observational study was conducted among 63 patients who were admitted with DNSI for a period of 18 months from December 2019 to June 2021 in the department of ENT, Government Medical College Thiruvananthapuram. Data collected using semi structured proforma was entered into Microsoft excel worksheet and were analyzed using SPSS software version 20.0.
Results: Men belonging to 5th and 6th decade were more affected.Submandibular space was the most commonly involved space, odontogenic infections being the most common etiology. Commonest organism was Streptococcus pyogenes. Incidence of complication was 46%, most common complication was airway narrowing (44.8%).
Conclusion: Deep neck space infection needs prompt diagnosis and appropriate treatment for good patient outcome.
Keywords: Deep neck space infection, Odontogenic, Bacteriology, Complication
INTRODUCTION
Deep neck space infections (DNSI) are bacterial infections in the potential spaces and fascial planes of the neck, either abscess formation or cellulitis.1 The complicated anatomical framework of the neck makes the process of diagnosis difficult.2 These bacterial infections originate from the upper aero digestive tract. They are severe, and if not treated adequately, may lead to death. Neck space infections can be divided into superficial and deep neck space infections. Superficial neck space infections are usually easy to treat. In contrast, deep neck space infections (DNSI) are difficult to diagnose;2 hence clinical suspicion is essential during the diagnosis as some of the deep neck infections are not evident on palpation. The incidence of this disease was relatively high before the advent of antibiotics, requiring prompt recognition and early interventions.3
The deep neck spaces that run the entire length of the neck include the retropharyngeal space, the danger space, the prevertebral space and the visceral vascular space. The spaces limited to above the hyoid include the submandibular space, the parapharyngeal space, the peritonsillar space, the masticator space and the parotid space. The potential space limited to below the hyoid is the anterior visceral space and suprasternal space. This area is enclosed by the middle layer of the deep cervical fascia and contains the thyroid gland, oesophagus and trachea.4
DNSI commonly follows infections like dental caries, tonsillitis, trauma to head and neck and in intravenous drug users; other sources may be from salivary glands, malignancies and foreign bodies. Odontogenic infection is one of the most common causes especially in developing countries.5 DNSI are usually polymicrobial in nature. Streptococci, Peptostreptococcus species, Staphylococcus aureus and anaerobes are the most commonly cultured organisms from DNSI.6 Serious life threatening complications are airway obstruction, pneumonia, lung abscess, sepsis, mediastinitis, pericarditis, internal jugular vein
thrombosis and carotid artery erosion.7 A delay in diagnosis or a missed diagnosis can even lead to death; therefore coping with deep neck infections remains a challenge to otolaryngologists even today. The aim of this study is to share experiences in terms of presentation, clinical trends, common sites, bacteriology, management, complications, and outcomes of deep neck space infections.
MATERIALS AND METHODS
This cross sectional study was conducted in Department of Otrhinolaryngology, Government Medical College Thiruvananthapuram from December 2019 to June 2021. Sixty three patients who were diagnosed to have deep neck space infections and treated in this institution were included in the study.
All patients fulfilling the selection criteria were explained about the purpose of study and a written consent was obtained from them to participate in the study before enrolment. Demographic data such as age, sex, address, detailed clinical history, general examination, ENT examination and systemic examination were done and recorded on predesigned proforma. Computerised Tomography scan of neck (CT) / Ultrasonography (USG) was done.
Empirical treatment was initiated with combination of Benzyl Penicillin, Gentamicin and Metronidazole as intravenous injections in appropriate doses and switched to appropriate antibiotics after obtaining culture and sensitivity reports. Anaerobic culture was not done and hence Metronidazole was given for a period of 5 days for all patients. Pus collected from patients who underwent surgical drainage was sent for microbiological studies and antibiotic sensitivity. Aerobic culture was done on MacConkey agar, blood agar and chocolate agar. Sensitivity was checked for commonly used drugs like Penicillin, Cephalosporin, Aminoglycosides, Cotrimoxazole, Ciprofloxacin and Erythromycin by using Kirby Bauer testing method. In cases with possibility of airway obstruction or aspiration tracheostomy was carried out. Patients were followed up at 1 week and 2 weeks of discharge
OBSERVATION AND RESULTS
63 cases of deep neck space infection from Department of Otorhinolaryngology, Medical College Trivandrum were studied during the period of December 2019 to June 2021.
Most of the cases of deep neck space infections belonged to 5th and 6th decade. The mean age of presentation was 50 years (± 15.9) (Figure1).
Out of 61 patients with deep neck space infections 69.1% were males and 38.1% were females. Increased prevalence was seen among males (Figure 2).
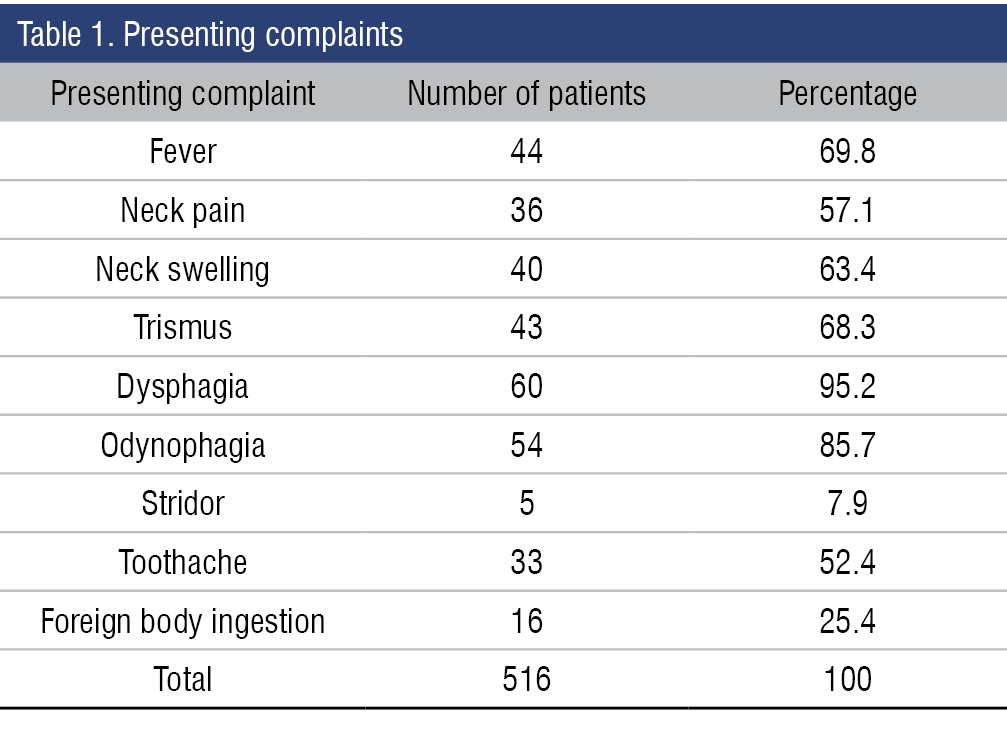
Dysphagia was the most common presenting complaint (95.2%) followed by odynophagia (85.7%), fever (69.8%), trismus (68.3%), neck swelling (63.4%), neck pain (57.1%), toothache (52.4%), foreign body ingestion (25.4%), stridor (7.9%) (Table 1).
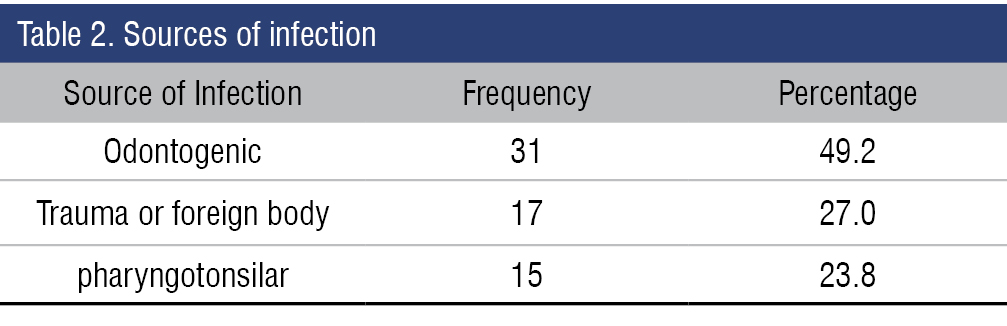
The most common aetiology was odontogenic seen in 31 patients (49.2%), followed by trauma or foreign body (27.0%) and pharyngotonsillar (23.8%). Among the 15 patients with infection of pharyngotonsillar origin 1 patient had histopathological report of squamous cell carcinoma (Table 2).
Single deep neck space involvement was seen in 32 patients (50.8%) and more than 1 space involvements were seen in 31 patients (49.2%). 43.7% had isolated retropharyngeal space involvement, 25% isolated peritonsillar, 22% isolated submandibular and 9.3% had isolated parapharyngeal space involvement.
Among 63 patients pus culture was sent and the common organism isolated in culture was Streptococcus pyogenes (22.2%). Klebsiella pneumoniae (14.2%) and Pseudomonas aeuroginosa (11.1%), 1 patient each isolated Enterococcus and MRSA. 46% of the cultures were sterile and 3.3% had mixed infection. 52% were culture positive were as 48% were culture negative. Streptococcus pyogenes species isolated were 84.6% sensitive to Penicillin, 69.2% sensitive to Gentamicin. Patients with Penicillin resistance were given 3rd generations
Cephalosporin (Cefotaxim). Pseudomonas aeruginosa isolated were 100% sensitive to Gentamicin. Enterococcus was 100% sensitive to Ampicillin and Penicillin. Klebsiella isolated were 100% sensitive to Amikacin and Gentamicin. MRSA was sensitive to Linezolid and Vancomycin. Among 63 patients 29 (46%) had complications. Airway narrowing was the most common complication encountered (44.8%) followed by mediastinal extension (34.4%), septicemia (17.2%), IJV thrombosis (17.2%), multi organ failure (10.3%), pneumonia (6.8%) and pleural effusion (3.4%). All patients with airway obstruction underwent tracheostomy. Among 63 patients there were 9(14.2%) deaths.
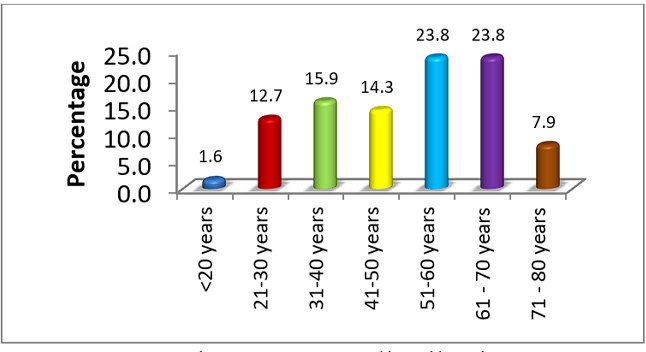
Figure 1. Age distribution
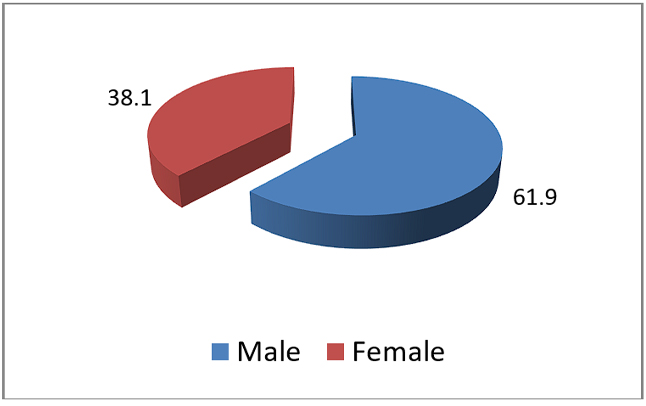
Figure 2. Sex distribution
DISCUSSION
According to this study, most of the patients with deep neck space infection (DNSI) belonged to 5th and 6th decades. 47.6% of patients belong to the age group. The mean age of presentation was 50 years. This varied in comparison with studies by Suehara et al (37.1 yrs),3 Gidley et al (25.5 yrs),9 Ridder et al (44.5 yrs),10 Miller et al (37.8 yrs),11 Lee et al (35.4yrs),13 Wang et al (41.8 yrs).8 The variation probably may be attributed due to non inclusion of paediatric population in the study. The gender comparison showed a definite predominance in males (F: M = 0.61). This is comparable with different studies like Panduranga Kammath et al14 (0.81), Lee et al(0.80),15 Abshirini H et al (0.82),16 Suehara et al(0.45),3 Har EI et al(0.71),12 John and MN (0.18)17 which unanimously showed a male preponderance.
In this study most common presenting complaint was dysphagia 60(95.2%), followed by odynophagia 54(85.7%) and fever 44(69.8%) similar to study by Sethi and Stanley20 where odynophagia (86%) was one among the most common symptoms. In most studies of deep neck space infection pain, neck swelling and fever are the most prevalent symptoms.5,3,4 Presenting complaints varied according to the space involved. In this study submandibular abscess and Ludwig‘s angina most commonly presented with neck swelling whereas patients with retropharyngeal and parapharyngeal space involvement mostly presented with dysphagia. 5 patients presented with stridor and underwent emergency tracheostomy. Most of the patients had more than 1 complaint. The most common source of DNSI in this study was odontogenic (49.2%) which was similar to studies by Gujrathi et al,4 Suehara et al,l3 Huang et al.19 Association of dental caries with occurrence of submandibular abscess is statistically proven in this study. Foreign body or trauma was the cause for 17 patients (27 %). Among these 17, for 3 patients the direct cause for development of DNSI was not clear and it was thought possibly due to minor trauma which went unnoticed by the patients and all 3 of them were diabetic. Among 14 patients with foreign body ingestion history, 12 had retropharyngeal abscess.
Pharyngotonsillar origin was seen in 23.8%, of this 1 patient had histopathological report of squamous cell carcinoma. In the pre-antibiotic era, studies demonstrated that most (70-80%) deep neck infections resulted from complicated pharyngeal infections. A decreased incidence (9-16%) of pharyngotonsillar sites of origin has been recently described these were in studies by Lee et al.15 This change is also high lightened in this study (odontogenic 49.2% and pharyngotonsillar 23.8%).
Involvement of various spaces depends on the source of infection. In this study submandibular space was most commonly affected (51%) this may be because most common source of infection was dental caries. Ludwig‘s angina was observed in 45%. The results were in conjunction with studies by Suehara et al,3 Mathew et al.21 Multiple spaces involvement is considered as poor prognostic factor. Among 63 patients studied positive culture report was obtained in 52 % cases. Most common organism isolated in culture was Streptococcus pyogenes (22.2%) and then Klebsiella pneumoniae (14.2%) and Pseudomonas aeuroginosa (11.1%). 46% of the cultures were sterile. This may be because of the prior intake of antibiotics before admission. This is similar to study by Lin et al.22 In 4 samples anaerobic organism was detected but no growth was not observed, due to lack of better anaerobic culture methods in our institution. The microbiology of deep neck infections changes with time 56. Contemporary reports from different countries or areas may reveal different common pathogens.
The difference in the etiology of the infection may be a contributing factor. For example, intravenous drug abuse, mandibular fractures and skin infections were common causes of deep neck infections in the report by Parhiscar and Har-El.18 This may explain why Staphylococcus epidermidis and S. aureus played a significant role in their study (28% and 22% of positive cultures, respectively). The difference between the distributions of the involved spaces in the different reports is another contributing factor. Streptococcus species isolated were 84.6% sensitive to Penicillin, 69.2% sensitive to Gentamicin, patients with Penicillin resistance were given 3rd generations Cephalosporin (Cefotaxim). Klebsiella isolated were 100% sensitive to Amikacin and Gentamicin. Pseudomonas aeruginosa isolated were 100% sensitive to Gentamicin. Enterococcus was 100% sensitive to Ampicillin and Penicillin. MRSA was sensitive to Vancomycin and Linezolid. This pattern of antibiotic sensitivity justifies the use of combination of Benzyl Penicillin, Gentamicin and Metronidazole as empirical therapy. Further changes were made according to culture and sensitivity reports. In this study the complication rate was (29 among 63 patients) 46% and the most frequent complication was airway narrowing (44.8%) followed by mediastinitis (34%), sepsis (17%). Special attention should be given to airway management when patients present with trismus or signs of upper airway obstruction, particularly in Ludwig‘s angina, in which there is gross oedema of the floor of mouth and of the anterior tongue due to bilateral submandibular, sublingual and submental space infections. For all patients with airway narrowing tracheostomy was done. Apart from this 13 patients, 12 other patients underwent tracheostomy because of anticipated intubation difficulty due to trismus. Parh iscar et al18 analyzed 210 patients with neck abscesses and reported a need for tracheostomy under anaesthesia in 44% of cases, which demonstrates the severity of this condition. Adequate management of airways with intubation using flexible fibroscopy and or a tracheostomy in cases of significant trismus and oedema of the tongue is a priority in the initial approach to DNSI. A tracheal intubation with rigid laryngoscopy may be difficult in these patients due to the possibility of distortion in the airway anatomy, tissue rigidity, and a limited access to the mouth. Thus, tracheostomy must always be considered whenever there is respiratory difficulty. Sometimes attempting intubations can worsen an already damaged airway.5 The complication rates in various studies were; Suehara et al3 (12.5%), Sethi and Stanley (19%)20 The increase in rate of complication in this study may be due to delay in presentation during the COVID pandemic period. In this study there were 9 deaths of which 5 were due to septicemia and were presented late to the institution, 5 of them had COVID infection, of which 4 of them had multiple co-morbidities belonging to the age group of more than 60 years and one 28 year old patient whose cause of death was meningitis following head injury. Hence from this study DNSI patients with co morbidities who developed COVID infection have poor prognosis. In this study, complications were more among diabetic patients. Also in patients between 30-50 years and it is statistically proven this may be because all of them had other associated co-morbidities.
CONCLUSION
63 cases of Deep neck space infection were studied and the following conclusions were made:
- Deep neck space infection was common among men in 5th to 6th decades.
- The most common source of DNSI was odontogenic.
- Submandibular space was most commonly involved.
- Streptococcus pyogenes was the most common organism isolated.
- Upper airway narrowing followed by mediastinitis, were the most commonly encountered complications.
- Deep neck space infection has high morbidity and mortality rates, particularly when associated with septicaemia / COVID infection.
End Note
Author Information
- Dr Anjali Vinod
Junior Resident, Department of Otorhinolaryngology, Government Medical College, Thiruvananthapuram - Dr Pramod Menon
Additional professor,
Department of otorhinolaryngology,
Government Medical College, Thiruvananthapuram - Dr. Satheesh S
Professor and HOD,
Department of Otorhinolaryngology,
Government Medical College, Kollam
Conflict of Interest: None declared
REFERENCES
- Huang T-T, Liu T-C, Chen P-R, Tseng F-Y, Yeh T-H, Chen Y-S. Deep neck infection: Analysis of 185 cases. Head Neck. 2004 Oct;26(10):854–60.
[Pubmed] - Almutairi D, Alqahtani R, Alshareef N, Al ghamdi YS, Al-Hakami HA and Algarni M. Deep Neck Space Infections: A Retrospective Study of 183 Cases at a Tertiary Hospital. Cureus. 12(2):e6841.
[Pubmed] | [Crossref] - Suehara AB, Gonçalves AJ, Claret Alcadipani FAM, Kavabata NK, Menezes MB. Deep neck infection - analysis of 80 cases. Brazilian Journal of Otorhinolaryngology. 2008 Mar;74(2):253–9.
[Pubmed] | [Crossref] - Gujrathi AB, Ambulgekar V, Kathait P. Deep neck space infection – A retrospective study of 270 cases at tertiary care center. World Journal of Otorhinolaryngology - Head and Neck Surgery. 2016 Dec 1;2(4):208–13.
[Pubmed] | [Crossref] - Priyamvada S, Motwani G. A Study on Deep Neck Space Infections. Indian J Otolaryngol Head Neck Surg. 2019 Oct;71(S1):912–7.
[Pubmed] | [Crossref] - Kataria G, Saxena A, Bhagat S, Singh B, Kaur M, Kaur G. Deep Neck Space Infections: A Study of 76 Cases. Iran J Otorhinolaryngol. 2015 Jul;27(81):293–9.
[Pubmed] - Yang S-W, Lee M-H, Lee Y-S, Huang S-H, Chen T-A, Fang T-J. Analysis of Life-Threatening Complications of Deep Neck Abscess and the Impact of Empiric Antibiotics. ORL. 2008;70(4):249–56.
[Pubmed] | [Crossref] - Wang L-F, Kuo W-R, Tsai S-M, Huang K-J. Characterizations of lifethreatening deep cervical space infections: A review of one hundred ninety-six cases. American Journal of Otolaryngology. 2003 Mar;24(2):111–7.
[Pubmed] | [Crossref] - Gidley P, Ghorayeb B, Stiernberg C. Contemporary management of deep neck space infections. Otolaryngology - Head and Neck Surgery. 1997 Jan;116(1):16–22.
[Pubmed] | [Crossref] - Ridder GJür, Technau-Ihling K, Sander A, Boedeker CC. Spectrum and Management of Deep Neck Space Infections: An 8-Year Experience of 234 Cases. Otolaryngol Head Neck Surg. 2005 Nov;133(5):709–14.
[Pubmed] | [Crossref] - Miller WD, Furst IM, Sàndor GKB, Keller MA. A Prospective, Blinded Comparison of Clinical Examination and Computed Tomography in Deep Neck Infections. Laryngoscope. 1999 Nov;109(11):1873–9.
[Pubmed] | [Crossref] - Har-El G, Aroesty JH, Shaha A, Lucente FE. Changing trends in deep neck abscess. Oral Surgery, Oral Medicine, Oral Pathology. 1994 May;77(5):446–50.
[Pubmed] | [Crossref] - Lee J-K, Kim H-D, Lim S-C. Predisposing Factors of Complicated Deep Neck Infection: An Analysis of 158 Cases. Yonsei Med J. 2007;48(1):55.
[Pubmed] | [Crossref] - Panduranga Kamath M, Shetty AB, Hegde MC, Sreedharan S, Bhojwani K, Padmanabhan K, et al. Presentation and management of deep neck space abscess. Indian J Otolaryngol Head Neck Surg. 2003 Oct;55(4):270–5.
[Source] - Lee J-K, Kim H-D, Lim S-C. Predisposing Factors of Complicated Deep Neck Infection: An Analysis of 158 Cases. Yonsei Med J. 2007;48(1):55.
- Abshirini H, Alavi S, Rekabi H, Hosseinnejad F, Ghazipour A, Yavari M, et al. Predisposing Factors for the Complications of Deep Neck Infection. Iranian Journal of Otorhinolaryngology. 2010 Jul 1;22.
[Source] - John S, Mn KR. Neck Space Infections: Clinical and Bacteriological Profile. 2018;(7):6.
- Parhiscar A, Har-El G. Deep Neck Abscess: A Retrospective Review of 210 Cases. Ann Otol Rhinol Laryngol. 2001 Nov;110(11):1051–4.
[Pubmed] - Huang T-T, Tseng F-Y, Liu T-C, Hsu C-J, Chen Y-S. Deep neck infection in diabetic patients: Comparison of clinical picture and outcomes with nondiabetic patients. Otolaryngol Head Neck Surg. 2005 Jun;132(6):943–7.
[Pubmed] | [Crossref] - Sethi DS, Stanley RE. Deep neck abscesses – changing trends. J Laryngol Otol. 1994 Feb;108(2):138–43.
[Pubmed] | [Crossref] - Mathew GC, Ranganathan LK, Gandhi S, Jacob ME, Singh I, Solanki M, et al. Odontogenic maxillofacial space infections at a tertiary care center in North India: a five-year retrospective study. International Journal of Infectious Diseases. 2012 Apr;16(4):e296–302.
[Pubmed] | [Crossref] - Lin C, Yeh F-L, Lin J-T, Ma H, Hwang C-H, Shen B-H, et al. Necrotizing Fasciitis of the Head and Neck: An Analysis of 47 Cases: Plastic and Reconstructive Surgery. 2001 Jun;107(7):1684–93.
[Pubmed] | [Crossref]